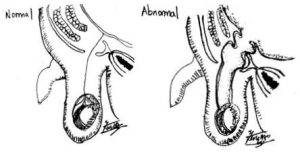
We were told by a doctor that our son has a hydrocele. Is a hydrocele dangerous?
A hydrocele contains fluid, and may present as discoloration and swelling of the scrotum. It is due to a patent opening and tract (patent processus vaginalis) that extends from the tummy to the groin or genitalia, but this opening is smaller than that seen in an inguinal hernia. A primary hydrocele can be communicating due to an open tract, or non-communicating (the opening is closed, but the fluid production exceeds the absorption, resulting in an accumulation of fluid). A secondary hydrocele is due to other causes which needs to be excluded for example infection, tumour or torsion of the testis.
When is the best time to repair paediatric hydroceles?
The best time to repair a primary hydrocele is classically advocated after 1 years old, but the evidence is not consistent(1). This is because the opening in the tummy closes by itself and fluid is reabsorbed by the body. This is often seen in communicating hydroceles noted from birth.
A hydrocele that is first noticed in a child or adolescent is different and may be a non-communicating hydrocele or secondary to an underlying problem. A secondary hydrocele needs to be explored and repaired at the earliest possible time.
Can oral medicine treat a hydrocele?
No medicine can cure a hydrocele. Surgery is needed to repair the opening of the tract, and drain the fluid.
What happens during the repair of a hydrocele in a child?
In a child, the surgery to repair a hydrocele is similar to the repair of an inguinal hernia. If the child is fit, I advise a laparoscopy to visualize both inguinal openings. There is up to 50% of patients who have a concurrent patent opening and tract on the other side of the tummy(2). When there is a patent opening on the other side of the tummy, it evolves into a hernia in 5 to 20% of patients in the future(3). I discuss with the parents the nature, benefits and risks of the procedure. The parents and patient decide whether they want a repair of the other side to prevent undergoing a second anaesthesia in future.
A laparoscopic repair can be performed if there are bilateral hydroceles. Under general and local anaesthesia, the incision is made within the umbilicus to insert the laparoscopic instruments. The opening(s) in the groin is then repaired. The instruments are removed and the wounds are closed with absorbable stitches. If there are reasons against a laparoscopic hydrocele repair, I perform the operation via an open technique.
For the open hydrocele repair, a groin skin crease incision is made, the opening and tract are repaired. The wound is closed with absorbable stitches.
For both laparoscopic and open techniques, when there is a need to examine the testis, an additional scrotal incision may be needed. In the repair, the fluid is drained and the tract is repaired.
How is the recovery after a hydrocele repair?
Your child goes home on the same day. Minimal bleeding is expected from the wound. Oral antibiotics is taken to prevent wound infection. The patient can have normal baths. Painkillers may be required for the first 3 days. In babies, it is advisable to change the diapers 2 to 3 hourly to keep the wound clean. A scab forms over the wound normally in the first 2 weeks and drops off with time. Some swelling may occur in the scrotum or genitalia after surgery and is the normal body reaction after surgery. This resolves by 6 weeks.
Risks of the hydrocele repair are infection, recurrent scrotal swelling, damage to the testis, ascending testis and repeat surgery. Infection presents as pain, redness, swelling, warmth and abnormal discharge of the wound site(s). If any of these complications occur, treatment is available and your doctor should be consulted early. It is important to avoid swimming and exercise for 3 weeks to allow the wound to have good healing and strength.
Are there alternatives to hydrocele repair?
Monitoring and waiting for the hydrocele to resolve by itself is an option. This is less likely when the patient is older than 2 years old. The warning signs of complications occurring are pain, increasing swelling, or change in colour of the scrotum or groin, and vomiting.
References
1. Chen Y, Wang F, Zhong H, et al. A systematic review and meta-analysis concerning single-site laparoscopic percutaneous extraperitoneal closure for pediatric inguinal hernia and hydrocele. Surg Endosc. 2017 Dec;31(12):4888–901.
2. Jin Z, Wang F. Effectiveness of Laparoscopy in the Treatment of Pediatric Hydrocele: A Systematic Review. J Laparoendosc Adv Surg Tech A. 2018 Dec;28(12):1531–9.
3. Esposito C, Escolino M, Turrà F, et al. Current concepts in the management of inguinal hernia and hydrocele in pediatric patients in laparoscopic era. Semin Pediatr Surg. 2016 Aug;25(4):232–40.
Share if you like this post
If you have other enquiries on children’s surgical conditions, feel free to contact us
© Copyright- 2025 Paediatric Surgery and Urology International
All Rights Reserved